AWS Public Sector Blog
4 ways AWS can help with Medicaid unwinding
Beginning on April 1, 2023, state Medicaid agencies (SMA) will have one year to “unwind” temporary COVID-era changes and return to pre-pandemic ways of working. A major part of that will be re-verifying that all 91 million members still qualify to receive Medicaid benefits.
For nearly a year, Amazon Web Services (AWS) has supported SMAs with in-house Medicaid expertise to identify unwinding issues and develop solutions to address them. The top four concerns that SMAs have shared are in approaching outreach and engagement, staffing shortages, returned mail, and reporting capabilities.
Cloud technology can help support and transform these areas. Read on to learn how AWS can help states across the country overcome these challenges across different scenarios.
1. Outreach and engagement
Agencies engage with members through physical mail; however, it’s been three years since SMAs have done outreach about enrollment, and many members may have different addresses than those on file.
Due to the scale of unwinding efforts, automation and scalable digital engagement is essential for successful unwinding efforts. Automated outreach to members through text and phone can not only inform members about their re-determination needs, but also collect the information necessary to conduct Medicaid renewals.
Consider an example scenario: Martha, a Medicaid beneficiary, moved in with her parents during the pandemic. If her SMA engages with her solely through physical mail with the address they have one file, Martha could lose coverage.
Scenario 1: The Medicaid agency sends a letter to Martha’s house using the address they have on file. Unfortunately, that’s her old address — remember, she moved in with her parents during the pandemic. She misses the letter and doesn’t respond in time.
Not receiving a letter and not providing an updated address may cause many Americans to lose their Medicaid coverage.
Amazon Pinpoint, a multi-channel communications tool, can help in this scenario. It uses automated texts and emails to help customers perform outreach — even collecting address information to complete a Medicaid renewal. Using Amazon Pinpoint, SMAs can support their members in retaining coverage.
Transformed Scenario 1: The Medicaid agency texts Martha to verify her address. Her address on file is incorrect, so Martha texts back her new address. She receives a confirmation text instructing her to anticipate a letter in the mail. Now, the Medicaid agency knows how to reach Martha and Martha knows to look for the letter. Plus, if she forgets to fill the letter out and send it back, she’ll get an automated reminder message.
2. Workload, staffing, and contact center coverage
With Medicaid agencies contacting all their members, and potential news coverage highlighting the impact of the unwinding, call contact centers may be overwhelmed with calls.
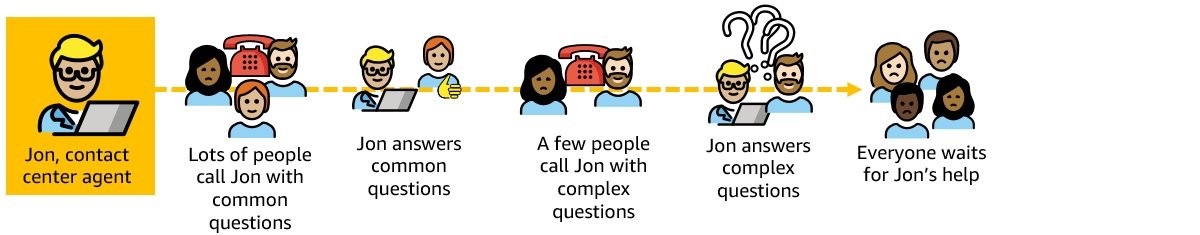
Consider another example scenario: Jon, a Medicaid contact center agent, fields questions from calling members and assists members through the renewal process. His passion is in helping members get coverage. However, if Jon spends majority of his time answering the same simple and common questions, he will spend less time making sure people are covered.
Scenario 2: Jon fields questions from calling members and assists members through the renewal process. A majority of the calls he answers are common questions and answers, which means callers in need of his expertise for more complex use cases must wait on hold until he can get to them. When he does, another dozen calls come into his queue.
Without automation, contact centers can maintain long wait times, with an increasing backlog of questions from members concerned about filing all the right paperwork to get their Medicaid coverage renewed.
Amazon Connect, Amazon Kendra, and Amazon Lex can help. Amazon Connect can answer and route calls, Amazon Kendra uses natural language processing to produce highly accurate answers, and Amazon Lex uses natural language models to speak directly to callers in multiple languages. An SMA can use these services to develop a highly accurate and scalable chatbot to assist Jon with his workload.
Transformed Scenario 2: Jon logs into his worker portal and sees an AWS powered bot has already answered 10 calls. The bot routes him specific calls that need his expertise. After working with the caller, Jon sees the bot has answered and resolved another five calls, with one more routed to his queue.
3. Returned mail
A critical focus of the public health emergency (PHE) unwinding is the challenge Medicaid agencies may face with regards to returned mail. The biggest implication of returned mail is members losing coverage because information from the state never reached them.
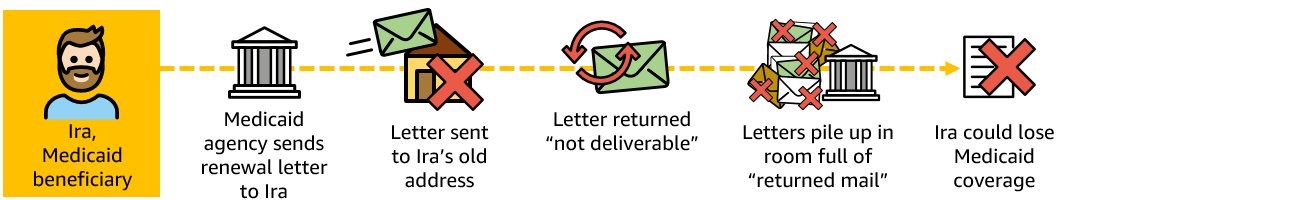
Consider another example scenario: Ira, a current Medicaid enrollee, was enrolled in June 2020 due to job loss, but he has since moved multiple times.
Scenario 3. The Medicaid agency sends a letter to Ira using the address they have on file from 2020, but the letter is returned for the reason, “Not Deliverable As Addressed – Unable to Forward (UTF).” The returned letter is added to a pile of other returned mail at the Medicaid agency. Ira is not contacted and may potentially lose Medicaid coverage.
SMAs do not have resources to manually process returned mail. Members should not lose Medicaid coverage because of returned mail.
AWS can help transform and automate the returned mail process through Amazon Textract and Amazon Pinpoint. Amazon Textract extracts data from forms such as letters, applications, and renewal documents with a high degree of accuracy. Amazon Pinpoint can use that extracted information to send customized text and email messages to the right person at the right time.
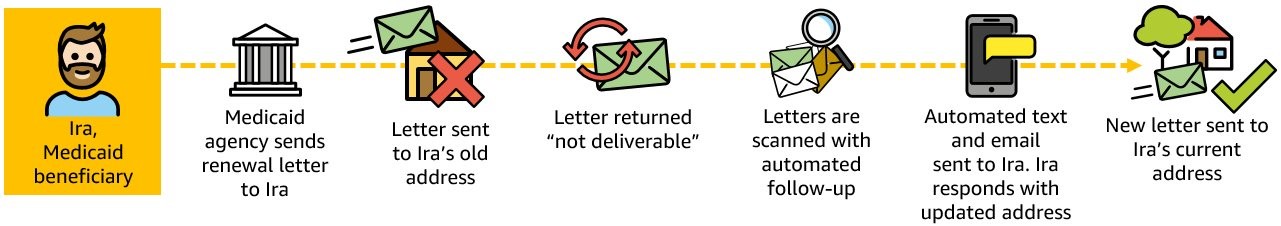
Transformed Scenario 3: The Medicaid agency sends a letter to Ira using the address they have on file from 2020, but the letter is returned for the reason, “Not Deliverable As Addressed – Unable to Forward (UTF).” An agency worker scans the returned mail. Amazon Textract reads the scanned file and extracts data. That extracted data can serve multiple uses. For example, Amazon Pinpoint can leverage that data to text and/or send an email to Ira. Ira responds to the email, providing an updated address. The Medicaid agency can now use the updated address to resend the renewal form to Ira’s current address.
4. Reporting
On April 1, 2023, the Centers for Medicare and Medicaid Services (CMS) will require states to report on specific metrics described in the “Unwinding Eligibility and Enrollment Data Reporting Template.” These metrics are designed to demonstrate a state’s progress towards restoring timely application processing, and initiating and completing renewals of eligibility for all Medicaid and Children’s Health Insurance Program (CHIP) enrollees.
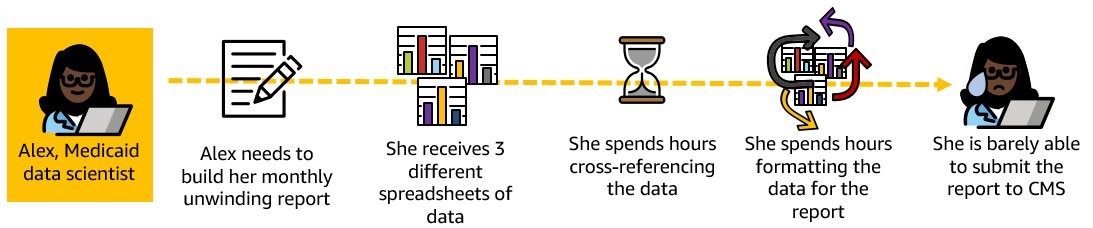
Consider another example scenario: Alex, a data analyst for the Medicaid agency, is responsible for submitting a report to CMS on the eighth day of every month. Alex must gather together data from the state’s eligibility system, fair-hearing system, and mail room. She then must verify the data is accurate, combine it together, and submit it to CMS.
Scenario 4: On the first day of each month, Alex gets three different data reports from the eligibility system, fair-hearing system, and mail room. She manually reviews each report and then attempts to combine the reports together. Because each report contains different data elements, she has to manually cross-reference data to combine it. She just barely gets the report compiled and submitted, but is bracing to repeat this manual process next month.
Manual reporting is not only challenging and time consuming, but can increase the risk of errors and hinder timely submission.
AWS can help transform this workflow with AWS Lake Formation and Amazon Quicksight. Lake Formation helps build a data lake in days and quickly import data from all your data sources. QuickSight empowers users to meet varying analytic needs from the same source of truth through modern interactive dashboards and paginated reports.
Transformed Scenario 4: Alex has created a data lake to ingest raw data from the three data sources. Additionally, she automated the generation of a dashboard from the relevant data elements in the data lake. On the first of each month Alex reviews the reporting dashboard and exports a .CSV file to submit by the deadline.
Conclusion
AWS is ready to support Medicaid agencies as they transform to meet PHE unwinding efforts. Contact the AWS Public Sector Team to learn more.
Health and human services (HHS) agencies across the country are using the power of AWS to unlock their data, improve citizen experience, and deliver better outcomes. See more Health and Human Services Cloud Resources here. Learn more about how governments use AWS to innovate for their constituents, design engaging constituent experiences, and more at the AWS Cloud for State and Local Governments hub.
All icons and emojis designed by OpenMoji – the open-source emoji and icon project. License: CC BY-SA 4.0
Read related stories on the AWS Public Sector Blog:
- Supporting state agencies with Medicaid unwinding outreach: Creating a multi-lingual two-way messaging system
- How public sector agencies can identify improper payments with machine learning
- Delivering better Medicaid services (and happier teams) with the AWS Cloud
- Using AI to rethink document automation and extract insights
Subscribe to the AWS Public Sector Blog newsletter to get the latest in AWS tools, solutions, and innovations from the public sector delivered to your inbox, or contact us.
Please take a few minutes to share insights regarding your experience with the AWS Public Sector Blog in this survey, and we’ll use feedback from the survey to create more content aligned with the preferences of our readers.